Transperforational Approach to Stent Closure of Duodenal Perforation
by Felix Boehme1*, Sebastian Roka2, Herbert Vedovelli1, Mary-Rose Reithofer1, Maximilian Kutschera3, Christian Sebesta1
1 Second Department of Internal Medicine, Klinik Donaustadt, Vienna, Austria
2Department of Surgery, Klinik Donaustadt, Vienna, Austria
3Science Center Donaustadt, Vienna, Austria
*Corresponding Author: Felix Boehme, Second Department of Internal Medicine, Klinik Donaustadt, Vienna, Austria
Received Date: 05 February 2026
Accepted Date: 10 February 2026
Published Date: 12 February 2026
Citation: Boehme F, Roka S, Vedovelli H, Reithofer MR, Kutschera M, et al. (2026) Transperforational Approach to Stent Closure of Duodenal Perforation. Ann Case Report 11: 2528. DOI: https://doi.org/10.29011/2574-7754.102528
Abstract
Duodenal perforations are potentially life-threatening emergencies requiring prompt intervention. Various etiologies, including Crohn’s disease and iatrogenic injuries, may underlie this condition. We report the case of a 44-year-old woman with long-standing Crohn’s disease who developed duodenal perforation following emergency colectomy. After the failure of surgical closure, a novel endoscopic transperforational technique using a fully covered Self-Expanding Metal Stent (SEMS) was successfully applied. This case highlights the versatility of endoscopic methods in complex anatomical scenarios and supports the use of self-expanding stents as a viable alternative in high-risk surgical patients.
Keywords: Stent-Closure; Duodenal Perforation; Crohn’s Disease; Transperforational Approach.
Introduction
Duodenal perforations are serious gastrointestinal emergencies requiring rapid treatment. Etiologies include inflammation, ulcers, malignancies, and iatrogenic trauma following surgical or endoscopic procedures [1]. Traditionally, treatment has focused on surgical repair, which may pose considerable risks, particularly in multimorbid patients [2]. In recent years, minimally invasive alternatives such as fully covered self-expanding metal stents (SEMS) have gained traction. These facilitate endoscopic bridging of the perforation site, significantly reducing the risk of peritoneal contamination and subsequent peritonitis [3]. Although initially used for other indications-such as anastomotic leakage or stricturesSEMS have been increasingly adopted for the management of gastrointestinal perforations [4].
Case Presentation
A 44-year-old woman presented to the emergency department with abdominal pain, diarrhea, and weight loss. She had a 25-year history of Crohn’s disease with colonic involvement and significant fistulizing behavior. Disease management was complicated by comorbid paranoid schizophrenia, which led to poor insight, refusal of immunosuppressive therapy, and persistent avoidance of surgical interventions. At presentation, she was without specific treatment, self-managing with a spelt-based diet.
Following admission to the Department of Gastroenterology, she repeatedly declined disease-specific therapy. Several weeks later, her condition deteriorated, with severe abdominal pain, peritonitis, hypotension, and elevated inflammatory markers. CT imaging revealed a complex colonic perforation. Emergent surgery was performed. In addition to colonic perforation, four entero-enteric fistulas were detected, one of which involved the duodenum.
Subtotal colectomy and creation of a terminal ileostomy were performed. The fistula was treated by excision, and the defect was closed with single-stitch sutures. Postoperatively, she was managed at the ICU and quickly transitioned to the general ward.
Despite multiple subsequent interventions, surgical repair of the duodenal perforation remained unsuccessful, necessitating continued negative pressure abdominal wound closure (NPAWT). An interdisciplinary decision between gastroenterology and surgery led to an endoscopic attempt for defect closure.
During a scheduled NPAWT change in the OR, gastroscopy with transpyloric placement of a SEMS was planned. After the removal of NPAWT and with the abdomen open, the gastroscope was inserted into the stomach without difficulty. Passage through the pylorus was hindered by inflammation and severe mucosal edema at the duodenal bulb. Initial attempts to access the descending duodenum were unsuccessful. With manual external splinting, duodenal passage was eventually achieved. In the D2 lumen was nearly obliterated due to local inflammation, and immediate desufflation through the perforation prevented proper visualization of the mucosa. With an externally placed metallic clip, the perforation could eventually be identified.
After successful guidewire insertion (0.035’’) into the duodenum, a 140 × 20 mm fully covered SEMS (Taewong Medical, TTS) was advanced through the working channel. However, due to sharp angulation at the pylorus and duodenal bulb, stent deployment failed. A second attempt using a near-the-scope wire-guided technique also proved unsuccessful.
At this point, the therapeutic strategy was modified intraoperatively. Using the delivery system externally, the perforation site was probed, and the stent was advanced into the distal duodenum. Full deployment was achieved, with the proximal end of the stent protruding several centimeters through the perforation site. Using external manual guidance, the gastroscope was reintroduced and retroflexed from the duodenal side through the perforation (Figure 1). A foreign body forceps was used to grasp the proximal stent suture and reposition the stent proximally, thereby bridging the defect completely. The NPAWT system was then reapplied.
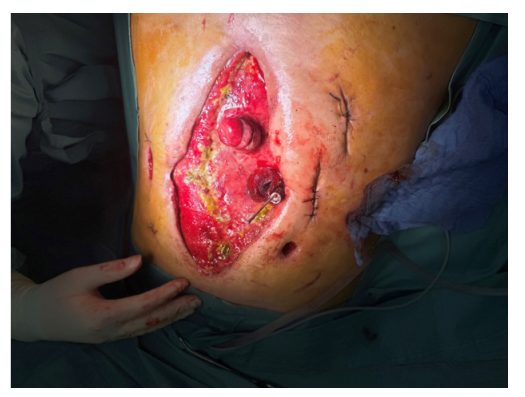
Figure 1: Intraprocedural situation: The proximal orifice of the deployed stent extents through the perforation. The endoscope and grasping forceps are introduced from above.
Contrast swallow studies the following day showed no residual leakage. The patient gradually resumed oral intake with fluids and soft diets and began nutritional buildup, while the NPAWT was changed regularly until closure of the abdominal wound.
Discussion
The management of duodenal perforations, particularly in high-risk or surgically complex patients, remains a significant challenge. This case demonstrates the potential role of endoscopic techniques, especially SEMS, in managing such complications when conventional surgical approaches are unsuccessful or contraindicated.
Anatomical constraints-such as inflammatory stenosis and duodenal angulation-can complicate stent placement. These obstacles are frequently encountered in patients with chronic inflammatory bowel disease. However, the adaptability of the endoscopic approach enabled an adjusted technique incorporating external stent placement and retrograde endoscopic repositioning. The technique utilized essentially a transperforational rendezvous approach required interdisciplinary coordination and creative problem solving, underscoring the importance of adaptability in minimally invasive endoscopic therapy.
Numerous studies have illustrated the effectiveness of SEMS in managing leaks and perforations in the upper GI tract [5,6]. SEMS placement, compared to surgery, may reduce morbidity, facilitate earlier resumption of oral intake, and shorten hospital stay [3]. However, complications such as stent migration, secondary leaks, and granulation tissue formation remain important considerations and should be systematically evaluated in follow-up protocols.
This case further supports the notion that SEMS may be a valuable alternative for duodenal perforations in selected patients. It also highlights the importance of innovation and interdisciplinary collaboration when standard interventions fail. Although not a standard-of-care procedure, this approach may offer a life-saving option in otherwise treatment-refractory cases.
Conclusion
This case report demonstrates that fully covered SEMS can be used even in technically challenging duodenal perforations where standard endoscopic stenting techniques fail. Although not likely to become standard practice, the described approach illustrates how unconventional endoscopic strategies can yield successful outcomes. These methods should be reserved for carefully selected cases in which conventional treatments have been exhausted.
References
- Nehra A, Godara R. (2019). The management of duodenal perforation: change over time. A case series and literature review. Hellenic Journal of Surgery. 91: 159-164.
- Bergström M, Arroyo Vázquez J, Nsouli G, Park PO. (2015). Good results of stent treatment in perforated duodenal ulcer. Lakartidningen. 112.
- Arroyo Vázquez JA, Khodakaram K, Bergström M, Park PO. (2021). Stent treatment or surgical closure for perforated duodenal ulcers: a prospective randomized study. Surgical Endoscopy. 35: 7183-7190.
- Wang X, Qu J, Li K. (2020). Duodenal perforations secondary to a migrated biliary plastic stent successfully treated by endoscope: case report and review of the literature. BMC Gastroenterology. 20: 149.
- Saito K, Ishikawa Y, Kitahara M, Nomura S, Fujisawa M, et al. (2024). Novel rendezvous technique for covered metal stent placement using balloon-assisted endoscope in duodenal perforation. Endoscopy. 56: E420-E421.
- Ferm S, Fisher C, Hassam A, Rubin M, Kim SH, et al. (2018). Primary endoscopic closure of duodenal perforation secondary to biliary stent migration: a case report and review of the literature. Journal of Investigative Medicine High Impact Case Reports. 6: 2324709618792031.
© by the Authors & Gavin Publishers. This is an Open Access Journal Article Published Under Attribution-Share Alike CC BY-SA: Creative Commons Attribution-Share Alike 4.0 International License. Read More About Open Access Policy.