Tracheocutaneous Fistula Formation Following Tracheostomy in a Patient with Motor Neuron Disease: A Case Report
by Majed Ibrahim Ahmed Hakami*
Department of Medicine, Pulmonology and Sleep Medicine Consultant, King Fahd Central Hospital, Jazan, Saudi Arabia
*Corresponding Author: Majed Ibrahim Ahmed Hakami, Department of Medicine, Pulmonology and Sleep Medicine Consultant, King Fahd Central Hospital, Jazan, Saudi Arabia
Received Date: 07 October 2025
Accepted Date: 13 October 2025
Published Date: 15 October 2025
Citation: Hakami MIA. (2025). Tracheocutaneous Fistula Formation Following Tracheostomy in a Patient with Motor Neuron Disease: A Case Report. Ann Case Report. 10: 2429. DOI:10.29011/2574-7754.102429
Abstract
We present the case of a young woman with diabetes mellitus and motor neuron disease who developed a tracheocutaneous fistula following tracheostomy performed for type 2 respiratory failure. Shortly after the initial tracheostomy, the patient experienced cardiopulmonary arrest requiring resuscitation and re-intubation. Bronchoscopy and CT revealed a tracheal wall defect with paratracheal air collection, consistent with a tracheocutaneous fistula. This case highlights the risks associated with airway management in neuromuscular disease patients and the importance of a multidisciplinary approach to complex tracheostomy complications.
Keywords: Tracheostomy Complication; Tracheocutaneous Fistula; Motor Neuron Disease; Respiratory Failure; Case Report.
Introduction
Tracheostomy is commonly indicated in patients with neuromuscular diseases to provide long-term ventilatory support. However, complications such as tracheocutaneous fistula, though rare, can be life-threatening. In individuals with motor neuron disease (MND), factors such as poor tissue integrity, heightened infection risk, and impaired healing predispose them to procedural complications. We report a case of tracheocutaneous fistula formation following tracheostomy in a young woman with suspected MND.
Case Presentation
Patient Information
- Young female with a known history of diabetes mellitus (DM) and motor neuron disease (MND)/chronic inflammatory demyelinating polyneuropathy (CIDP).
- Bedridden for two months prior to presentation.
- Initial Presentation
- Referred from a secondary hospital with decreased consciousness and oxygen desaturation.
- Arterial blood gas (ABG): pH 7.164, pCO₂ 130 mmHg - consistent with type 2 respiratory failure.
- Initially managed with BiPAP, but no significant improvement noted.
- CT brain revealed ischemic changes in bilateral preinsular regions.
Clinical Findings
- Upon arrival at the emergency department, the patient was intubated and placed on mechanical ventilation (PRVC settings: 45/5/14/380).
- Hemodynamically stable without vasopressor support.
- Glasgow Coma Scale (GCS): 8 (E4V1M3); pupils 2 mm, sluggishly reactive to light.
- Urine analysis suggested urinary tract infection; intravenous piperacillin-tazobactam (Tazocin) was initiated.
Tracheostomy and Complication
Date: 29/01/2024
- An elective tracheostomy using a 7.5 mm tube was performed.
- Approximately 15 minutes post-procedure, the patient developed bradycardia and cyanosis, followed by cardiac arrest.
- Cardiopulmonary resuscitation (CPR) was initiated per protocol and continued for 15 minutes.
- The patient was re-intubated following resuscitation.
Subsequent Management
- Continued on mechanical ventilation (FiO₂ 60%, PEEP 8).
- Maintained good urine output; remained afebrile.
- Follow-up ABG showed respiratory alkalosis: pH 7.5, pCO₂ 28 mmHg, HCO₃ 21 mEq/L; ventilator settings were adjusted accordingly.
Bronchoscopy and CT Findings
Bronchoscopy revealed a tracheal tear on the posterior wall with a tracheocutaneous fistula measuring approximately 2 cm (Figure 1).
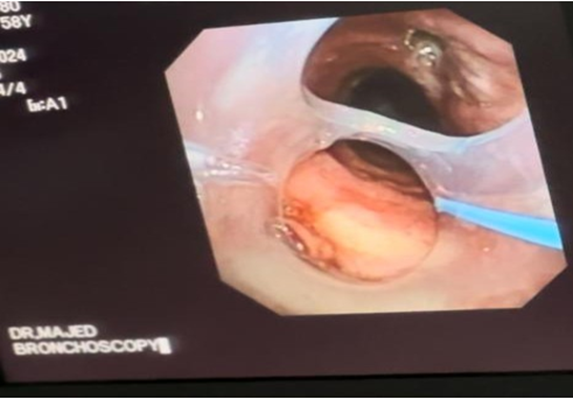
Figure 1: Bronchoscopy showing a posterior tracheal wall defect with a tracheocutaneous fistula measuring approximately 2 cm.
CT neck and chest with IV contrast showed
- A focal tracheal wall defect (7 × 9.5 mm) on the right posterolateral aspect at the level of the previous tracheostomy with paratracheal air collection (Figure 2).

Figure 2: Contrast-enhanced CT scan of the neck demonstrating a focal tracheal wall defect (7 × 9.5 mm) on the right posterolateral aspect with associated paratracheal air-filled cystic lesion.
- Associated paratracheal air-filled cystic lesion measuring 13 x 10 x 17 mm, suggestive of tracheal diverticulum or injury.
- Collapse consolidation in the left lower lobe (LLL) and right middle lobe (RML), with retained secretions in mainstem bronchi (more on the left).
- Bilateral ground-glass opacities and patchy consolidations, particularly in the posterior segment of the right lower lobe, consistent with aspiration pneumonia.
- Bilateral pleural effusions, more on the left.
- No evidence of pneumomediastinum or pneumothorax.
- Near-total sinus opacification, likely due to retained secretions (intubation-related).
- ETT and NGT in situ, and central line in right external jugular vein.
Outcome
- A successful repeat tracheostomy was performed on 22/02/2024.
- Postoperative oxygen saturation was maintained, and the patient remained stable on ventilatory support.
- She required prolonged ICU admission.
- During the ICU stay, she developed healthcare-associated infections that progressed to sepsis and ultimately septic shock.
Discussion
Tracheocutaneous fistula is an uncommon but recognized complication of tracheostomy. It typically results from prolonged mechanical ventilation, local infection, tissue ischemia, or procedural trauma [1,2]. In this patient, early post-tracheostomy cardiac arrest may have compromised tissue perfusion, leading to ischemic injury and fistula formation [3].
Recent literature emphasizes structured perioperative strategies for managing TCF. Selby et al. [4] highlighted the importance of preoperative bronchoscopy, tailored surgical closure techniques, and vigilant postoperative care. Wu et al. [5] proposed a decision-making algorithm for TCF repair, incorporating fistula size, soft tissue condition, and comorbidities. In complex cases, specialized flap closure techniques have shown durable outcomes [6], and multimodal strategies involving biodegradable material and flap grafting have been successful [7].
Risk factors such as smoking, malignancy, and prolonged tracheostomy duration have been identified as contributors to persistent fistula formation [8]. Our case also highlights the unique vulnerability of patients with neuromuscular disease. Impaired soft tissue support, prolonged immobility, and infection risk compound the likelihood of post-tracheostomy complications.
The CT findings in our case confirmed a localized tracheal defect with adjacent paratracheal air collection, consistent with contained perforation rather than free mediastinal air. Concurrent findings of aspiration pneumonia, pleural effusions, and bilateral collapse further underscore the complexity of management in such high-risk patients.
Broader scoping reviews of tracheostomy complications also highlight posterior wall injury, infection, and ventilator-associated complications, reinforcing the need for a multidisciplinary approach including pulmonologists, intensivists, ENT, and surgical teams [9].
Conclusion
Tracheostomy in patients with neuromuscular disease carries a substantial risk of complications, including tracheocutaneous fistula and tracheal injury. Timely imaging with CT scan aid in early detection and characterization of structural airway defects. Vigilant post-operative monitoring and prompt multidisciplinary intervention are essential to minimize morbidity and improve outcomes in this high-risk population.
Patient Consent
Written informed consent for publication of this case report and accompanying clinical details was obtained from the patient’s legal guardian, her son. Documentation of this consent is retained by the authors.
References
- Liao C, Zhao W, Zhou S, et al. (2017). Management of tracheocutaneous fistula after tracheostomy: A clinical review. Int J Otolaryngol. 2017: 1-7.
- Marchese S, Corrado A, Scala R, Corrao S, Ambrosino N, et al. (2010). Tracheostomy in ventilator-dependent patients: A multicenter survey. Respir Care. 55: 1062-8.
- Miller RG, Jackson CE, Kasarskis EJ, England JD, Forshew D, et al. (2009). Practice parameter update: The care of the patient with amyotrophic lateral sclerosis. Neurology. 73: 1218-26.
- Selby JN, Javia L, Goyal N. (2024). Perioperative management of tracheocutaneous fistula closure: A narrative review. J Oral Maxillofac Anesth. 3: 18.
- Wu C, Xu Y, Chen S. (2020). Surgical strategies and decision algorithm for persistent tracheocutaneous fistula repair: A retrospective review. J Thorac Dis. 12: 1741-51.
- Yoshida T, Sato H, Tanaka K, Watanabe Y, Umehara T. (2020). Successful closure of a large persistent tracheocutaneous fistula using skin flaps: A case report. Case Rep Otolaryngol. 2020: 1-4.
- Li H, Zhang Y, Liu J, Tang R. (2020). Large tracheocutaneous fistula successfully treated with bronchoscopic intervention, biodegradable material, and flap grafting. Front Med (Lausanne). 7: 278.
- Shin J, Lee H, Kim Y, et al. (2021). Risk factors associated with persistent tracheocutaneous fistula after decannulation: A systematic review. Otolaryngol Head Neck Surg. 164: 1110-8.
- Swain SK. (2025). Complications of tracheostomy: A scoping review. Airway. 8: 1-12.
© by the Authors & Gavin Publishers. This is an Open Access Journal Article Published Under Attribution-Share Alike CC BY-SA: Creative Commons Attribution-Share Alike 4.0 International License. Read More About Open Access Policy.