The Evolution of Integrated System Market Shaping: Navigating Financialization, Digital Transformation, and Strategic Governance in Emerging Health Economies
by Hala AlMossawi1, Neeraj Kak2*
1Associate Professor, Oklahoma State University, USA
2Public Health Advisor, AQUITY Global Inc, USA
*Corresponding author: Neeraj Kak, Public Health Advisor, AQUITY Global Inc, USA
Received Date: 17 March, 2026
Accepted Date: 23 March, 2026
Published Date: 26 March, 2026
Citation: AlMossawi H, Kak N (2026) The Evolution of Integrated System Market Shaping: Navigating Financialization, Digital Transformation, and Strategic Governance in Emerging Health Economies. J Community Med Public Health 10: 562. DOI: https://doi.org/10.29011/2577-2228.100562
Abstract
For over three decades, market shaping has been the cornerstone of global health, successfully driving down the prices of essential commodities like vaccines and antiretrovirals. However, as emerging economies transition from aid-dependency to domestic financing, the paradigm must shift from product affordability to integrated system governance. This paper proposes the Integrated System Market Shaping (ISMS) framework to address five interacting domains: macroeconomic drivers, strategic purchasing, private capital expansion, digital ecosystems, and regulatory stewardship. Through case studies of India, Indonesia, the Philippines, Kenya, and Brazil, we analyze the structural risks of healthcare financialization—in which private equity-backed consolidation often leads to staffing cuts and worse clinical outcomes—alongside the transformative potential of AI-driven strategic purchasing. We find that while remittances provide a critical private liquidity stream, they often exacerbate out-of-pocket vulnerability in the absence of formal risk pooling. The paper concludes with evidence-based recommendations for governing digital infrastructure as a publicinterest utility and for integrating public health safeguards into reimbursement models to ensure that rising prosperity translates into equitable health gains.
Keywords: Market Shaping; Integrated System Market Shaping (ISMS); Private Equity; Health Financing; Digital Transformation; Antimicrobial Resistance; Remittances; Emerging Economies
Introduction
The landscape of global public health is currently undergoing an unprecedented structural transformation, shifting from a historical focus on commodity affordability to the more complex challenge of governing integrated health ecosystems. For over three decades, the concept of market shaping was largely synonymous with correcting failures in the pharmaceutical and vaccine sectors. Early interventions, such as the Blue Circle social marketing initiative in Indonesia during the 1970s and 1980s, used branding, price subsidies, and private retail networks to stimulate demand for essential health products such as condoms and oral rehydration salts (Legowo, G. F. 1991; Ezizika, O et al 2021). These successes paved the way for a more sophisticated generation of global commodity pricing strategies, where coordinated donor financing revolutionized markets for antiretroviral therapy, reducing prices for first-line treatments by more than 99 percent between 2000 and 2020 (WHO, 2025; World Bank, 2025a).
However, empirical evidence suggests that these product-focused successes are being overtaken by broader systemic shifts in emerging economies. Countries are transitioning away from a reliance on external aid toward domestic financing models characterized by rising middle-class incomes, substantial remittance liquidity, and the rapid digitalization of health infrastructure. This evolution is accompanied by the accelerating financialization of service delivery, where private equity (PE) firms and global asset managers consolidate fragmented provider networks into corporate chains, often prioritizing financial returns over clinical outcomes. Consequently, the traditional paradigm of market shaping must evolve into a framework of Integrated System Market Shaping (ISMS) that governs ownership structures, data ecosystems, and provider incentives alongside commodities.
The Conceptual Framework for Integrated System Market Shaping (ISMS)
Understanding the modern health economy in emerging markets requires a multidimensional analytical lens. The ISMS framework identifies five interacting domains:
- Macroeconomic Drivers: GDP growth and urbanization shift demand toward tertiary care, attracted by remittance flows that function as informal social insurance.
- Health Financing and Strategic Purchasing: Moving from passive reimbursement to active, value-based contracting that rewards quality over volume.
- Service Delivery Markets and Private Capital: Governing the entry of PE and institutional investors to prevent “stealth consolidation”.
- Digital Ecosystems and Information Governance: Treating digital health data as a public utility to prevent proprietary monopolies.
- Regulatory and Stewardship Architecture: Safeguarding competition and patient safety through antitrust and clinical audits.
Each domain creates feedback loops. For example, when high remittance liquidity meets a consolidated private provider market, it can inadvertently trigger price inflation if strategic purchasing capacity is weak.
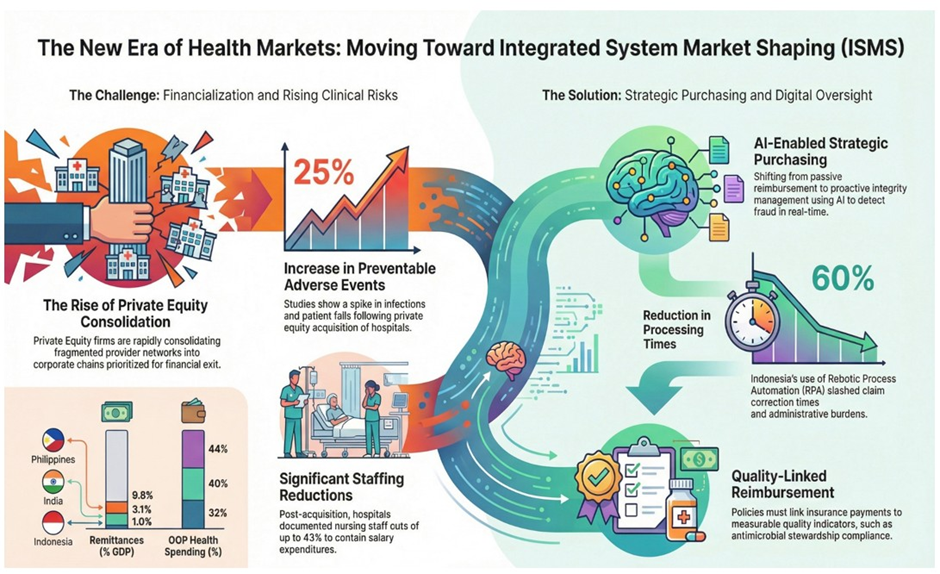
Figure 1: Remittance Flows and Out-of-Pocket Health Spending: The Double-Edged Sword of Emerging Market Healthcare.
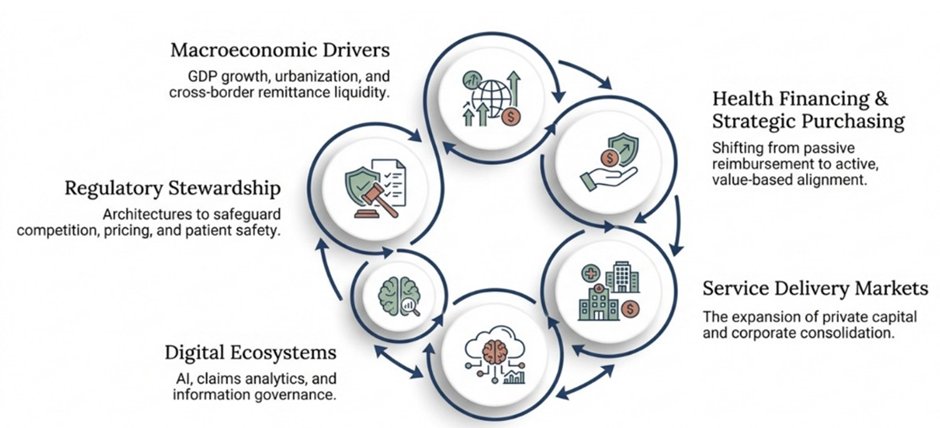
Figure 2: The Integrated System Market Shaping (ISMS) framework across five interdependent domains
Macroeconomic Determinants and the Remittance Nexus
The economic foundation of health systems in several emerging economies is increasingly anchored in cross-border labor mobility. Officially recorded remittances to LMICs reached nearly $700 billion in 2024, a 10% growth from the previous year (World Bank, 2025b; Migration Data Portal, 2025). In India, remittances in 2024 reached an estimated $137 billion, while in the Philippines, these flows account for 9.8% of GDP (World Bank, 2025b).
While these inflows enhance household resilience, they are unevenly distributed. Families with migrant members often bypass public queues for private specialty services, reinforcing the concentration of hospital capacity in urban centers. The lack of risk-pooling mechanisms contributes to high out-of-pocket (OOP) expenditure, which remains as high as 70% in Nigeria (WHO, 2025; OECD, 2025) (Table 1).
|
Country |
Remittances (% GDP) |
OOP Health Spending (% of Total) |
Current Trends |
|
Philippines |
9.8 |
44 |
High reliance on remittances for tertiary care |
|
Nigeria |
6.2 |
70 |
Chronic underfunding of public systems |
|
Kenya |
3.5 |
27 |
Mobile payment integration (M-Pesa) for care |
|
India |
3.1 |
40 |
Rapid growth of PE-backed corporate hospital chains |
|
Indonesia |
1.0 |
32 |
Transitioning from aid recipient to Gavi donor |
Table 1: Remittances, Out-of-Pocket Health Spending, and Current Healthcare Trends in Selected Emerging Markets.
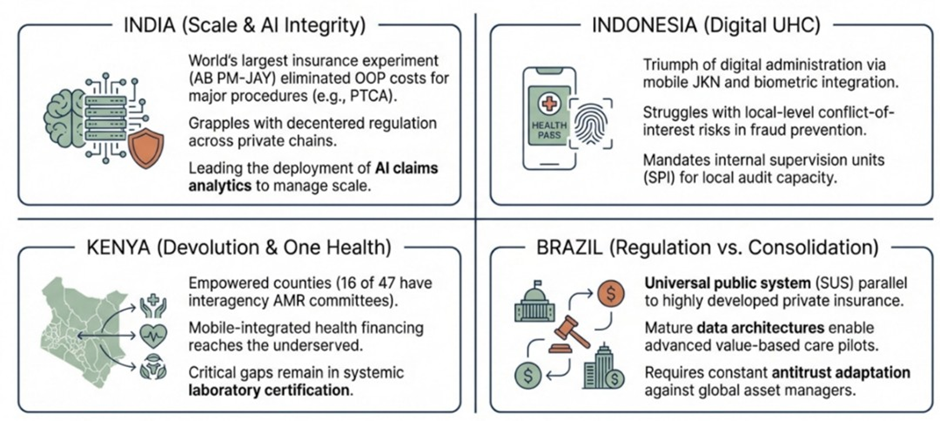
Figure 3: Emerging economies offer diverse blueprints for navigating system transitions and shaping markets.
The Financialization of Service Delivery and Private Equity Expansion
As remittance liquidity stabilizes, PE firms have identified healthcare in emerging markets as a high-margin target for capital deployment. Global healthcare PE deal value reached record highs in 2025 (Bain & Company, 2026). This trend is characterized by the corporatization of medicine, using leveraged buyouts (LBOs) in which clinical entities are purchased with debt collateralized by the hospital’s own assets (Fuse Brown & Hall, 2024).
Clinical Risks and Staffing Cuts
Evidence suggests that PE acquisition is frequently followed by aggressive cost-cutting. Hospitals have been documented to reduce physician staffing by 19% and nursing staff by 43% post-acquisition (American Progress, 2024). Harvard researchers found that patient deaths in emergency departments increased by 13% at PE-acquired hospitals, a finding directly linked to these staffing reductions (HMS, 2023). Furthermore, inpatient wards saw a 25% increase in preventable adverse events, including a 38% increase in infections following central line placements (NIH, 2024) (Table 2).
|
Investment Type |
Description |
Strategic Goal |
|
Leveraged Buyout (LBO) |
Acquisition using high debt collateralized by target assets |
Maximizing equity returns through debt servicing |
|
Add-on Acquisition |
Purchase of smaller entities by a platform company |
Market power and economies of scale (Serial acquisitions) |
|
Growth Investment |
Capital injection for expansion in mature companies |
Revenue growth and margin improvement before exit |
|
Real Estate Investment Trust (REIT) |
Sale-leaseback of hospital land and buildings |
Asset stripping to provide immediate investor dividends |
Table 2: Key Private Equity Investment Strategies in Healthcare.
Digital Transformation: AI and Strategic Purchasing
While financialization poses risks, digitalization offers powerful tools for ISMS. India’s National Health Authority (NHA) has pioneered the use of AI to shift from reactive fraud detection to “proactive integrity management” within the Ayushman Bharat scheme (PIB, 2025; JPMS, 2024). In Indonesia, BPJS Kesehatan has integrated robotic process automation (RPA) through RACE and RAPID platforms, reducing claim correction times from several minutes to under 97 seconds (Asian Business Review, 2025).
However, generative AI has also supercharged healthcare fraud. Authorities noted that deepfake-related fraud attempts surged by 3,000% in 2023 (TruthScan, 2025). This technological arms race requires that market shaping include robust digital integrity frameworks and mandatory algorithmic transparency (OECD, 2024a; OECD, 2024b) (Table 3).
|
Digital Intervention |
Purpose |
Documented Outcome |
|
NHA AI Claims Analytics (India) |
Real-time fraud management |
Shift to proactive integrity management |
|
RACE/RAPID RPA (Indonesia) |
Automation of claim entry/payment |
40-60% reduction in processing time |
|
JAPRI Generative AI (Indonesia) |
Internal knowledge management |
90% satisfaction; reduced HR/procurement burden |
|
Mobile JKN (Indonesia) |
Simplified administration |
Shorter waiting times; reduced OOP costs |
|
ABDM Unified Health System (India) |
Strategic purchasing confluence |
Improved data capture for DRG-based rates |
Table 3: Key Digital Health Interventions and Outcomes in India and Indonesia.
Infection Prevention and Antimicrobial Resistance: A Systemic Challenge
System market shaping must incorporate quality safeguards to address public health issues such as antimicrobial resistance (AMR), which contributes to 4.5 million deaths annually (WHO, 2025b). ARCH studies have revealed that LMICs have up to 20 times higher rates of bacterial colonization harboring resistant genes than in the US and Europe (CDC, 2024; MDPI, 2024). In Kenya, only 53.6% of assessed health facilities were able to perform cultures (GARDP, 2024). Strategic purchasing must move beyond price to link reimbursement to mandatory AMR reporting and hospital wastewater treatment standards (WEF, 2025; MTaPS, 2023) (Table 4).
|
Country |
National AMR Action Plan |
Diagnostic Culture Capacity |
IPC Integration in Reimbursement |
Key Gap / Priority |
|
Kenya |
Yes (2023–2027) |
Low (53.6% of facilities) |
Not yet linked |
Expand lab network; link AMR data to NHIF contracting |
|
India |
Yes (NAP-AMR active) |
Moderate (urban-rural gap) |
Partial (Ayushman Bharat DRG) |
Integrate AMR stewardship into ABDM data flows |
|
Indonesia |
Yes (in development) |
Low outside Java |
Not yet linked |
Leverage BPJS digital platform for IPC reporting mandates |
|
Philippines |
Yes (AMR-NAP 2019– 2023; renewal pending) |
Moderate (tertiaryconcentrated) |
Not yet linked |
Update NAP; link PhilHealth accreditation to IPC standards |
|
Brazil |
Yes (PNPCIRAS active) |
Moderate–High (SUS network) |
Partial (public sector only) |
Extend IPC requirements to private PE-owned hospital chains |
|
Sources: WHO Global AMR Surveillance Report (2025); GARDP Kenya AMR Report (2024); MTaPS Kenya Technical Brief (2023); Kenya NAP-AMR (2023–2027); Frontiers in Tropical Diseases (2025). |
||||
Table 4: AMR and Infection Prevention Readiness Indicators Across Selected Emerging Markets.
The Evolving Role of Global Donors and Health Partnerships
As countries graduate from Gavi support, they face the risk of a “graduation cliff.” In Vietnam, a rapid shift to localized financing led to a decline in childhood immunization rates from 87% to 77% due to stockouts (Immunization Economics, 2025). Gavi Phase 6 (2026–2030) now includes a “Catalytic phase” for middle-income countries to decouple programmatic support from vaccine subsidies,
ensuring sustainability (Gavi, 2025a). Simultaneously, the World Bank is working toward delivering quality care to 1.5 billion people by 2030 through government-endorsed “National Health Compacts” (World Bank, 2025c; Gavi-WBG, 2025).
Discussion
The findings of this paper suggest that the current era of health system development is defined by a “Double-Edged Sword” of financialization and digitalization.
- The Risk of the New Alpha: In the private equity domain, the “New Alpha” of investment must be redefined as accountability rather than just growth. The reliance on “dry powder”—currently exceeding $1 trillion globally in PE funds—exerts immense pressure on firms to find quick exits, often at the expense of primary care stability (Bain & Company, 2026; PE Stakeholder Project, 2024). The collapse of systems like Steward Health Care illustrates the systemic risk when clinical assets are stripped for dividends (Morning Brew, 2026). Emerging economies must implement “social licenses to operate” that mandate minimum staffing levels and capital reinvestment commitments (SHVS, 2025; Bipartisan Policy Center, 2024).
- The Digital Commons vs. Data Monopolies: Digital transformation has significantly improved efficiency, as seen in Indonesia’s 40–60% reduction in processing times (Asian Business Review, 2025). However, the “Decentred Regulation” model— where non-state actors like insurers and platforms help set rules— pluralizes oversight but can fragment norms (Lumarpub, 2024). Governments must resist the urge to let proprietary AI systems manage clinical triage, as algorithmic opacity can entrench market dominance and bias (OECD, 2024a).
- The Resiliency Trap: While remittances provide household-level resilience, they act as a “resiliency trap” that allows governments to underfund public risk-pooling. Without integrating these private flows into formal insurance platforms, the poor will continue to face 70% OOP expenditures, leading to medical poverty despite national GDP growth.
Evidence-Based Recommendations for Integrated System Market Shaping
The evolution from commodity-focused interventions to integrated system governance requires a new set of evidence-based policy priorities.
1. Strengthen Strategic Purchasing and QualityLinked Reimbursement
Governments should move beyond passive insurance toward active, value-based purchasing by:
- Implementing tiered reimbursement linked to accreditation, HAI rates, and antimicrobial stewardship.
- Integrating active cost surveillance tools into the digital infrastructure to reduce private sector bill inflation.
- Transitioning from fee-for-service to bundled payments or capitation models.
2. Enhance Regulatory Oversight of Private Capital
To counter the risks of financialization, regulators must increase transparency by:
- Enforcing mandatory ownership transparency to disclose PE or leveraged debt structures.
- Monitoring staffing levels and patient safety metrics postacquisition, imposing sanctions if quality drops.
- Updating competition and antitrust laws to prevent serial “stealth” acquisitions.
3. Govern Digital Infrastructure as a Public Interest Utility
Digitalization must be treated as a strategic public utility through:
- Enforcing interoperability mandates using standardized, open-source protocols to prevent data monopolies.
- Demanding algorithmic transparency and public auditing of AI tools used in claims and clinical triage.
- Investing in proactive integrity management via publicsector AI capacity for real-time fraud detection.
4. Integrate AMR and IPC into System Design
System market shaping must treat pathogen containment as a prerequisite for resilience by:
- Mandating AMR reporting linked to hospital licensing and insurance reimbursement.
- Investing in One Health infrastructure, such as wastewater treatment and automated diagnostic capacity, as common goods.
- Utilizing anticipatory governance and predictive modeling to identify infection transmission pathways.
5. Transition Donor Models toward System Stewardship
Global donors should align their exit strategies with long-term governance needs by:
- Using blended finance to de-risk private investment in underserved primary care regions.
- Supporting National Health Compacts that align health, finance, and labor ministries.
- Providing catalytic technical assistance for strategic purchasing and competition policy for graduating countries.
Conclusion
Over the past two decades, market shaping has delivered measurable gains by expanding access to affordable health commodities. Yet in emerging health economies today, the central challenge is no longer price alone, but the governance of increasingly complex health systems. Financialized provider markets, rapid digitalization, and rising antimicrobial resistance have fundamentally altered how health services are produced, financed, and delivered.
This reality requires a strategic shift from commodity-centric interventions toward Integrated System Market Shaping—one that aligns financing, regulation, and digital infrastructure around public objectives. Strategic purchasing, transparent ownership oversight, and accountable use of data must become core policy tools to ensure that private investment supports quality, safety, and equity rather than undermining them.
For governments and global partners, the policy imperative is clear: strengthening stewardship capacity is now as critical as mobilizing resources. Countries that invest early in integrated governance frameworks will be better positioned to translate economic growth and technological innovation into resilient, high-performing health systems. Those that do not risk entrenching inefficiency, widening inequality, and escalating public health threats. The future of health system performance will be shaped not by market forces alone, but by the policy choices that govern them.
To explore these dynamics across specific regional contexts, readers can access the System Market Shaping Interactive Intelligence Portal, which provides AI-driven simulations based on the data presented in this document.
References
- Legowo GF (1991) Blue Circle Campaign: A Study of Family Planning Campaign in Kebayoran Lama, South Jakarta, Indonesia.
- Ezezika O, Ragunathan A, El-Bakri Y, Barrett K (2021) Barriers and facilitators to implementation of oral rehydration therapy in low- and middle-income countries: A systematic review. PLoS One 16: e0249638.
- World Health Organization (2025) Most countries make progress towards universal health coverage, but major challenges remain, WHO–World Bank report finds.
- Advancing the World Bank Group Goal: Reaching 1.5 billion people with quality, affordable health services by 2030, accessed March 3, 2026.
- Fuse Brown EC, Hall MA (2024) Private Equity and the Corporatization of Health Care - Stanford Law.
- 5 Consequences of Private Equity’s Expansion in Health Care Services.
- Governing with Artificial Intelligence - OECD, accessed March 3, 2026.
- Ministry of Health and Family Welfare, Government of India (2025) NHA showcases use of artificial intelligence to strengthen transparency and integrity in India’s digital health ecosystem at CVC workshop.
- Remittances - Migration Data Portal, accessed March 3, 2026.
- Healthcare Private Equity Market 2025: Resurgence and Record..., accessed March 3, 2026.
- Global Healthcare Private Equity Report 2026 - Bain & Company, accessed March 3, 2026.
- Private Equity Healthcare Deals: 2024 in Review, accessed March 3, 2026.
- Regulating Financialization in the Healthcare System: A Toolkit for States - shvs.org, accessed March 3, 2026.
- Health Care Provider Consolidation - Bipartisan Policy Center, accessed March 3, 2026.
- The human cost of private equity’s healthcare boom - Morning Brew, accessed March 3, 2026.
- Deaths Rose in Emergency Rooms After Hospitals Were Acquired by Private Equity Firms, accessed March 3, 2026.
- Infections and falls increased in private equity-owned hospitals - NIH, accessed March 3, 2026.
- Full Report: Governing with Artificial Intelligence | OECD, accessed March 3, 2026.
- Strengthening India’s Healthcare System: Combating Fraud with Technology and Policy Reforms | Journal of Pioneering Medical Sciences, accessed March 3, 2026.
- BPJS Kesehatan Recognised at Indonesia Technology Excellence Awards, 2025.
- AI-Driven Fraud in Global Healthcare: 2025 Trends and Countermeasures | TruthScan, accessed March 3, 2026.
- A review of India’s AB-PM-JAY including strategic purchasing, decentralised regulation and financial risk protection, accessed March 3, 2026.
- Innovative Studies Investigate Spread of Antimicrobial Resistance in Communities and Hospitals - CDC, accessed March 3, 2026
- Assessment of Antimicrobial Resistance Diagnostic Capacity and Antibiotic Use in 10 Counties in Kenya - GARDP, accessed March 3, 2026.
- Stop playing catch-up with superbugs: the anticipatory governance of antimicrobial resistance - The World Economic Forum, accessed March 3, 2026.
- Global antibiotic resistance surveillance report 2025 - World Health Organization (WHO), accessed March 3, 2026.
- Gavi and World Bank Group Deepen Collaboration to Boost Health System Resilience and Regional Vaccine Manufacturing, accessed March 3, 2026.
- Phase 6 (2026–2030) - Gavi, the Vaccine Alliance, accessed March 3, 2026.
- Vietnam’s quick policy reversal highlights challenges in vaccine financing, accessed March 3, 2026.
- Kenya’s National Action Plan on antimicrobial resistance: measuring implementation progress - Frontiers, accessed March 3, 2026.
- Effective and Sustainable Governance Structures for Combating Antimicrobial Resistance at Health Facilities in Kenya - The Medicines, Technologies, and Pharmaceutical Services (MTaPs) Program, accessed March 3, 2026.
- Republic of Kenya (2023) National Action Plan on Prevention and Containment of Antimicrobial Resistance - Guidelines, Standards & Policies Portal.
- OECD (2025) Health expenditure in relation to GDP: Health at a Glance 2025 | OECD.
- OECD (2025) How artificial intelligence is accelerating the digital government journey – OECD.
© by the Authors & Gavin Publishers. This is an Open Access Journal Article Published Under Attribution-Share Alike CC BY-SA: Creative Commons Attribution-Share Alike 4.0 International License. Read More About Open Access Policy.