New Insights into the Anatomy of the Internal Iliac and Uterine Veins - A Cadaveric Study
Florian Nardin1*, Paula van Appeldorn1, Stefan Schneeberger2, Helga Fritsch1, Romed Hörmann1
1Institute of Clinical and Functional Anatomy, Medical University of Innsbruck, Austria
2Department of Operative Medicine, University Clinics for Visceral-, Transplantation- and Thoracic Surgery, Medical University of Innsbruck, Austria
*Corresponding author: Florian Nardin, Medical University of Innsbruck, Institute for Clinical-Functional Anatomy, Müllerstrasse 59, A-6020 Innsbruck, Austria
Received Date: 27 September, 2022
Accepted Date: 06 October, 2022
Published Date: 10 October, 2022
Citation: Nardin F, van Appeldorn P, Schneeberger S, Fritsch H, Hörmann R (2022) New Insights into the Anatomy of the Internal Iliac and Uterine Veins - A Cadaveric Study. J Surg 7: 1559. DOI: https://doi.org/10.29011/2575-9760.001559
Abstract
Little is known about the variable uterine veins and their draining into the internal iliac vein. This becomes relevant with the upcoming field of uterus transplantation. Detailed knowledge of the number and length of venous vessels is crucial for careful operation planning regarding the anastomosis location and dissection point. Using cadaveric donors, we extracted the pelvic organs and dissected the venous vessels starting from the inferior vena cava and ending at the uterine veins in the parametrium. We measured the length of the common iliac vein and the internal iliac vein until the first uterine vein’s orifice. The number of uterine veins and that of the parietal vessels were counted. We found a high variability of uterine vein numbers (1 to 7). A distinct plexus wasn’t reaching the internal iliac vein in most of the cases. The length of the internal iliac vein was measured with a mean of 38 mm.
Concluding, a suitable length for an anastomosis during uterus transplantation and sparing of a simultaneous y-graft extraction in cadaveric donation was found.
Keywords : Pelvic veins ; Uterine transplantation ; Uterine veins ; Y-graft
Abbreviations: V: Vein; A: Artery; SEM: Standard Error of The Mean; COM: Communis; Dext: Right; Sin: Left; Utx: Uterus Transplantation; IIV: Internal Iliac Vein; CIV: Common Iliac Vein; UV: Uterine Vein; EIV: External Iliac Vein; NS: Not Significant
Introduction
Uterine vein anatomy is, until now, poorly described in the literature. Nevertheless, the emerging field of Uterus Transplantation (UTx) requires a profound knowledge of the pelvic vessels to locate adequate dissection locations along the Internal Iliac Vein (IIV) or The Uterine Vein (UV). This location should offer an extensive and anatomically constant vessel for easier anastomosis and improved blood flow without the risk of occlusion. The uterine arteries were discussed in literature by several teams and with many techniques in the past. Even being subjected to a slight variability, they mostly emerge from the internal iliac artery, either directly, from the umbilical or the inferior gluteal artery. [1] The Common Iliac Vein (CIV) and its tributaries were also described in the literature, and a high variance was seen in all studies. A radiological survey by Shin et al. describes 19 variations between the CIV and the internal and External Iliac Veins (EIV) on both sides. [2] The uterus drainage is described as draining the venous blood through three systems: The first system uses anastomoses with the ovarian veins. Thus, the upper part of the uterine blood flows into the inferior vena cava directly or indirectly via the renal vein. Secondly, the uterovaginal plexus is thought to drain the lower part of the uterus blood into the uterine veins. Finally, the uterine veins drain the majority of venous outflow and merge into the IIV via the so called periuterine plexus. The uterine venous plexus is formed directly around the uterus and drains into one or more uterine veins in the cervical region of the uterus. [3] These veins are being described as two inconsistent veins, depending on their position to the oelvic ureter: a superficial one and a much larger deep UV. [4] These veins, which have no valves, dilate significantly during pregnancy becoming high-volume veins and are crucial for a proper uterine blood flow. [5] No details are described regarding the number of UVs or the exact confluence point with the IIV.
Therefore, we decided to conduct an anatomical study, focusing on the IIV and determining UVs’ exact location and number. Moreover, we aim to characterise the often-cited “plexus uterinus” in more detail. To our knowledge, we are the first to describe the exact number and location of UVs’ inflow into the IIV in a cadaveric study.
Material and Methods
In this cadaveric study started in January 2020 and terminated in July 2022 we used human bodies donated to the Institute of Clinical and Functional Anatomy of the Medical University of Innsbruck. All body donors had given their written informed consent prior to death for their use for scientific and educational purposes. All cadavers were preserved using an arterial injection of a formaldehyde solution and immersion in phenolic acid and water for one to three months [6]. The possibility of this solution causing morphological preservation artefacts can be denied. The bodies are a representative sample of the general female Austrian and German population at the age of death [7]. We investigated eighteen pelvic specimens. Three hemipelvices had to be excluded because of preceding vessel damage, causing possible bias in number and length on this side. So, we studied 33 hemipelvices in total. All pelvic organs, including vasculature, were removed from the pelvic bone for an optimal overview. The veins were dissected from the bifurcation of the inferior vena cava as far as possible into the parametrial tissue (Figure 1A and Figure 1B). All side branches were dissected and rated as relevant when having a diameter of at least 3 mm. The length of the IIV was measured from the confluence of the IIV and EIV and the first vein diverging to the uterus. All UVs were counted, and the given anatomy was evaluated. Additionally, the number of parietal vessels leaving the IIV between the bifurcation and the first UV was noted. Many already published iliac vein variations were found during this dissection. [2] These were also noted. Three IIV had to be excluded from the statistical evaluation because of a doubled IIV (numbers 14-16 shown in Table 1).
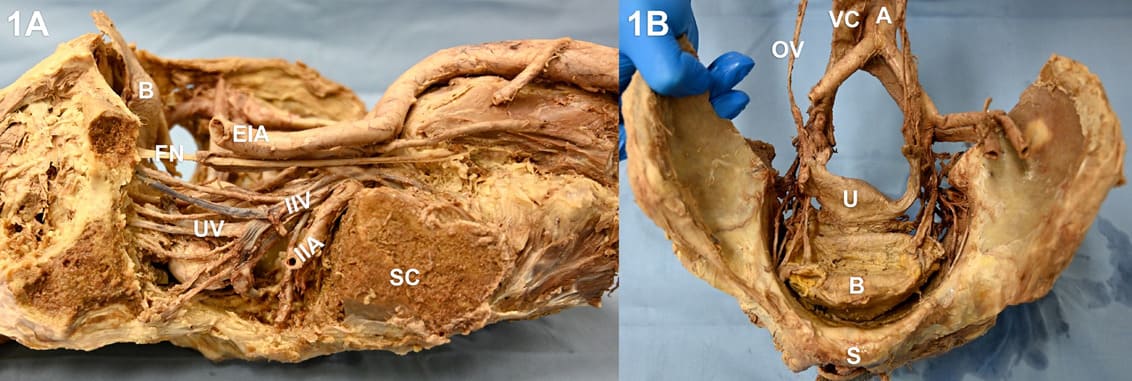
Figure 1: Overview of dissected samples, A: IIV and UV as seen from lateral, B: pelvic specimen seen from above, rectum as sacral bone removed (B: bladder, FN: femoral nerve, UV: uterine vein, IIV: internal iliac vein, IIA: internal iliac artery, EIA: external iliac artery, S: hip, U: uterus, OV: ovaric vessels, A: aorta).
|
Präp # |
v. iliaca com sin |
v. iliaca com dext |
v. iliaca interna sin |
v. iliaca interna dext |
# v. uterinae sin |
# v. uterinae dext |
# parietal vessels sin |
# parietal vessels dext |
|
1 |
87 |
49 |
48 |
64 |
1 |
1 |
1 |
1 |
|
2 |
92 |
34 |
44 |
32 |
3 |
5 |
5 |
5 |
|
3 |
67 |
53 |
48 |
46 |
3 |
2 |
2 |
2 |
|
4 |
73 |
63 |
45 |
14 |
1 |
4 |
4 |
1 |
|
5 |
NA |
40 |
NA |
28 |
NA |
3 |
NA |
2 |
|
6 |
90 |
51 |
26 |
NA |
3 |
NA |
1 |
NA |
|
7 |
75 |
46 |
29 |
48 |
3 |
1 |
0 |
5 |
|
8 |
88 |
63 |
18 |
23 |
2 |
3 |
1 |
1 |
|
9 |
68 |
55 |
60 |
0 |
3 |
7 |
6 |
1 |
|
10 |
77 |
28 |
32 |
61 |
4 |
4 |
2 |
2 |
|
11 |
NA |
NA |
84 |
83 |
1 |
1 |
NA |
4 |
|
12 |
87 |
49 |
27 |
50 |
2 |
2 |
2 |
4 |
|
13 |
57 |
49 |
42 |
NA |
5 |
NA |
3 |
NA |
|
14 |
85 |
52 |
2 |
55+21 |
4 |
3 |
0 |
1+2 |
|
15 |
80 |
53 |
27 |
38+25 |
3 |
5 |
4 |
2+2 |
|
16 |
98 |
67 |
34 |
47+37 |
3 |
4 |
2 |
1+2 |
|
17 |
58 |
49 |
30 |
36 |
1 |
2 |
0 |
4 |
|
18 |
95 |
48 |
11 |
50 |
3 |
3 |
3 |
1 |
Statistical analyses
Were performed in Microsoft® Excel® for Microsoft 365 MSO. A two-side T-test was done. A standard error of the mean (±) is provided for all calculated means.
Results
Table 1 shows the acquired measurements of the pelvic specimens. The CIV showed an average length of 64.4 mm (± 3.2), with a mean of 79.8 mm on the left side (± 3.1) and 49.9 mm (± 2.3) on the right side, respectively (p < 0.01). The IIV showed an average length of 38 mm (± 3.7) until the first uterine vein branch. The left IIV was 35.7 mm (± 4.6) and the right 41.2 mm (± 6.1) long. (p = ns). A classical plexus, defined as the confluence of more than four veins with multiple anastomoses in between them reaching the IIV, was found in 9 out of 33 cases (example shown in Figure 2A and Figure 2B). The mean number of UV branches entering the IIV was 2.8 (± 0.25) with a maximum of 7 and a minimum of 1. On the left side, there were in average 2.6, and on the right side in average 3.1 inflows. We found 2.9 small parietal branches between the confluence of the IIV and the EIV and the first UV; left: 2.2 (± 0.5), right: 2.5 (± 0.5). (p = ns) Moreover, nine variations of the iliac veins were found, of which two according to the scheme of Shin et al. [2] (Figure 2C and Figure 2D), including six anastomoses between IIV and EIV.
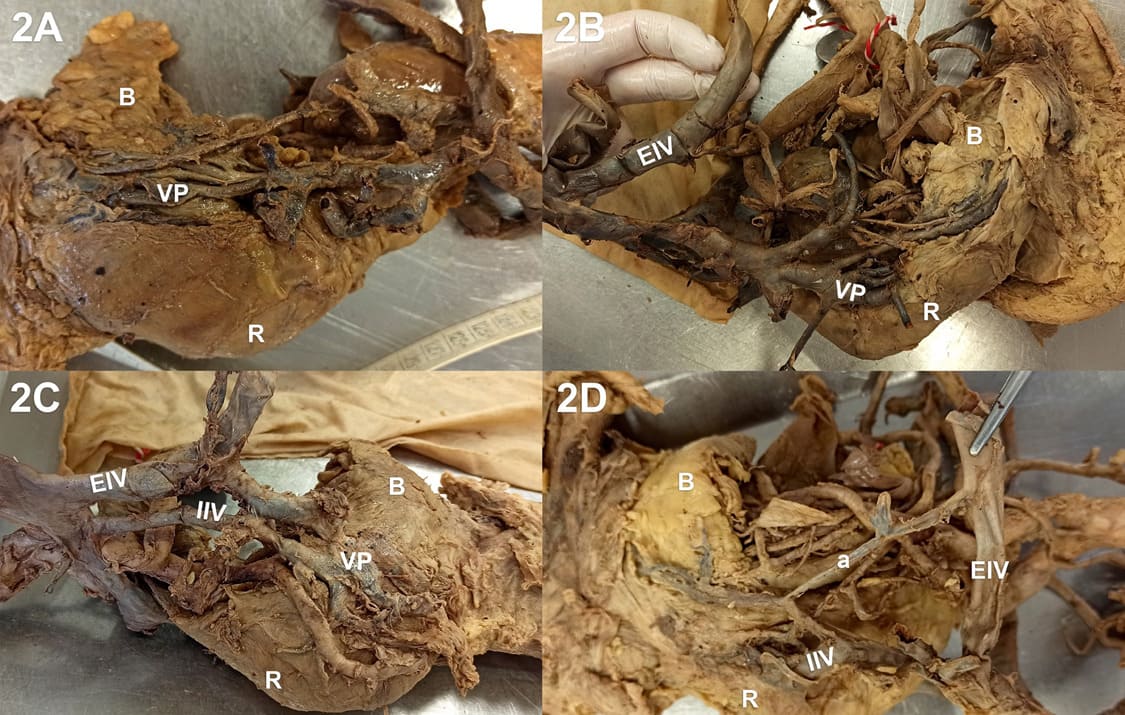
Figure 2: Examples of venous sitations: A: singular uterine vein insertion into the IIV, B: dilated IIV with multiple uterine vein insertions, C: variation of the IIV with high insertion in CIV, D: IIV-EIV anastomosis (B: bladder, VP: venous plexus, R: rectum, a: anastomosis, EIV: external iliac vein, IIV: internal iliac vein)
Discussion
Herein we aimed to characterise the confluence of the UV with the IIV and the general venous outflow of the uterus. UTx, as described by various teams before [8,9] is a field with considerable future potential. As such, the ideal workflow and technique have yet to be found. As described by the authors dealing with cadaveric and living donors [10-13], the venous retrieval for a promising anastomotisation of the uterus graft with the recipient’s vessels seems to be the most critical step during the surgery. Of course, the retrieval in living donors poses a remarkable higher risk and difficulty than in deceased donors because of the obligate sparing of the IIV. Nevertheless, the procedure remains challenging even in deceased donors. Therefore, an exact knowledge of the venous situation is crucial for proper planning of the surgery. Radiological imaging is not always available because of the urgent setting during a deceased donor explantation. Consequently, knowledge of the frequency and variations of UVs and their confluence with the IIV can be helpful. The mean of less than three venous branches shows that a plexus is seldomly reaching the IIV as described by many textbooks. Instead, more singular veins (Figure 1A) seem to drain into the IIV. This is underlined by our findings of nine plexus out of 33 samples.
The singular inflow of uterine veins into the internal iliac vein renders the venous anastomosis using the UVs feasible but more complex and time-consuming. This is the only possible way in a living donor operation and should be done by expert vascular surgeons. A retrieval with the internal iliac stump should be considered in the case of a deceased donor. Even if some variations are possible, they are far less frequent than the UVs’ variations. The IIV gives a suitable length with a mean of 38 mm for a successful anastomose with the recipients’ CIV. The variations of the iliac veins can affect the uterine outflow and have to be considered anyways and were described in detail before [2]. A further important consideration when explanting organs in multiorgan deceased donors has to be done on behalf of the y-graft. This vessel kit, consisting standardly of the aortal and vena cava bifurcation, is often needed for vessel reconstruction if an unexpected vessel situation of the liver or pancreas is given. [10] Also, parts of the iliac bifurcation can be used for vessel reconstruction [11,13]. For obtaining a suitable length without too many branches to ligate, which can potentially cause bleeding, therefore a knowledge of the iliac veins’ anatomy is crucial.
As a multiorgan donor is also an option for a uterus donation, we have two concurring organ systems that need an iliac vein graft. On the one hand, harvesting an intact y-graft should be prioritised, as it might be required for the proper reconstruction of vital organ vessels. On the other hand, adequate uterus retrieval needs a certain length of the IIV for a later anastomosis. Our findings may clarify that both organ needs can be satisfied. With over 3 cm of internal iliac vein length and less than three parietal branches between the iliac confluence and the first UV, including the first and biggest parietal branch, a sufficient anastomosis should be guaranteed for uterus graft as well as y-graft.
Even if Life Uterus Donation (LD) poses many advantages for transplantation, such as ideal antigen match, minimal ischemia time, and an optimal operation planning time, the most significant benefit is the possibility of performing a presurgical radiological evaluation of the vessels. The exact anatomy can be identified optimally through magnetic resonance angiography. [5,14] Described complications and Achilles’ heels of LD are often the variability of UVs’ number [15] and the retrieval of veins without damaging the donor’s ureters [16]. The UV was sometimes found unsuitable for proper venous outflow, and the ovarian or uteroovarian veins had to be used in these cases. [17,18] Therefore, knowing the anatomic variations, and with it the suitability of the UV, is even more important while planning the procedure in reguard to the decision which vessel can be ideally used for operation. The future of uterus transplantation will prove the suitability of contemporary uterus extraction and multiorgan donation and further successful LD.
References
- Liapis K, Tasis N, Tsouknidas I, Tsakotos G, Skandalakis P, et al. (2020) Anatomic variations of the uterine artery. Review of the literature and their clinical significance. Turk J Obstet Gynecol 17: 58-62.
- Shin M, Lee JB, Park S bin, Park HJ, Kim YS (2015) Multidetector computed tomography of iliac vein variation: prevalence and Surgical and Radiologic Anatomy 37: 303-309.
- Cicinelli E, Einer-Jensen N, Galantino P, Alfonso R, Nicoletti R (2004) The vascular cast of the human uterus: From anatomy to physiology.In: Annals of the New York Academy of Sciences. New York Academy of Sciences 2004: 19-26.
- Robin F, Dion L, Lavoue V, Goujon A, Boudjema K, et al. (2022) Relationship between uterine veins, ureter, and hypogastric nerve foruterine transplantation: An anatomic study. Clinical Anatomy 2022.
- Kristek J, Johannesson L, Novotny R, Kachlik D, Fronek J (2020) Human uterine vasculature with respect to uterus transplantation: Acomprehensive review. Vol. 46, Journal of Obstetrics and Gynaecology Blackwell Publishing 2020: 2199-2220.
- Platzer W, Putz R, Poisel S (1978) [New system for the preservation and storage of anatomical matter]. Acta Anat 102: 60-67.
- Konschake M, Brenner E (2014) “Mors auxilium vitae”-Causes of death of body donors in an Austrian anatomical department. Ann Anat 196: 387-393.
- Jones B, Saso S, Bracewell‐Milnes T, Thum M, Nicopoullos J, et al. (2019) Human uterine transplantation: a review of outcomes from the first 45 cases. BJOG 126: 1310-1319.
- Brännström M (2015) Uterus transplantation. Curr Opin Organ Transplant 20: 621-628.
- Guler N, Dayangac M, Yaprak O, Akyildiz M, Gunay Y, et al. (2013) Anatomical variations of donor portal vein in right lobe living donor liver transplantation: the safe use of variant portal veins. Transplant International 26: 1191-1197.
- Gałązka Z, Grochowiecki T, Nazarewski S, Rowiński O, Chudziński W,et al. (2006) A Solution to Organ Shortage: Vascular Reconstructions for Pancreas Transplantation. Transplant Proc 38: 273-275.
- Riederer BM, Bolt S, Brenner E, Bueno-Lopez JL, Cirulescu ARM, et (2012) The legal and ethical framework governing Body Donation in Europe – 1st update on current practice. Eur J Anat 16: 1-21.
- Dunn DL, Morel P, Schlumpf R, Mayoral JL, Gillingham KJ, et al. (1991) Evidence that combined procurement of pancreas and liver grafts does not affect transplant outcome. Transplantation 51: 150
- Testa G, Koon EC, Johannesson L, McKenna GJ, Anthony T, et (2017) Living Donor Uterus Transplantation: A Single Center’sObservations and Lessons Learned From Early Setbacks to Technical Success. American Journal of Transplantation 17: 2901-2910.
- Brännström M, Johannesson L, Bokström H, Kvarnström N, Mölne J, et al. (2015) Livebirth after uterus transplantation. The Lancet 385: 607-616.
- Brännström M, Dahm Kähler P, Greite R, Mölne J, Díaz-García C, et al. (2018) Uterus transplantation: A rapidly expanding field. Transplantation 102: 569-577.
- Chmel R, Novackova M, Janousek L, Matecha J, Pastor Z, et al. (2019) Revaluation and lessons learned from the first 9 cases of a Czech uterus transplantation trial: Four deceased donor and 5 living donor uterus transplantations. American Journal of Transplantation 19: 855-864.
- Wei L, Xue T, Tao KS, Zhang G, Zhao GY, et al. (2017) Modified human uterus transplantation using ovarian veins for venous drainage: the first report of surgically successful robotic-assisted uterus procurement and follow-up for 12 months. Fertil Steril 108: 346-356.
© by the Authors & Gavin Publishers. This is an Open Access Journal Article Published Under Attribution-Share Alike CC BY-SA: Creative Commons Attribution-Share Alike 4.0 International License. Read More About Open Access Policy.