Innovations in Chest Wall Reconstruction: A Critical Review
by Gabriel Lunardi Aranha1, João Paulo Cassiano de Macedo1*, Pedro Henrique Xavier Nabuco de Araujo2, José Ribas Milanez de Campos1, Ricardo Mingarini Terra2, Paulo Manuel Pêgo-Fernandes3
1 Instituto do Coracao, Hospital das Clinicas HCFMUSP, Faculdade de Medicina, Universidade de Sao Paulo, Sao Paulo, SP, BR.
2Instituto do Câncer do Estado de São Paulo (ICESP), Hospital das Clinicas de São Paulo, Faculdade de Medicina, Universidade de Sao Paulo, Sao Paulo, SP, BR.
3Full professor, Thoracic Surgery Division, at Instituto do Coracao, Hospital das Clinicas HCFMUSP, Faculdade de Medicina, Universidade de Sao Paulo, Sao Paulo, SP, BR.
*Corresponding Author: João Paulo Cassiano de Macedo, Instituto do Coracao, Hospital das Clinicas HCFMUSP, Faculdade de Medicina, Universidade de Sao Paulo, Sao Paulo, SP, BR.
Received Date: 12 February 2026
Accepted Date: 17 February 2026
Published Date: 19 February 2026
Citation: Aranha GL, Macedo JPC, Araujo PHXN, Campos JRM, Terra RM, Pêgo-Fernandes PM (2026) Innovations in Chest Wall Reconstruction: A Critical Review. J Surg 11: 11570 DOI: https://doi.org/10.29011/2575-9760.011570
Abstract
The chest wall is a complex and dynamic structure essential for protecting intrathoracic organs and maintaining respiratory mechanics. Defects resulting from oncologic resections, trauma, infections, congenital abnormalities, or surgical failures can severely compromise its function, leading to respiratory insufficiency, instability, herniation, and chronic infections. Robust reconstructive strategies are therefore imperative to restore anatomical integrity and support patient recovery. Indications for chest wall reconstruction are diverse, with primary etiologies including extensive oncologic resections aimed at achieving tumor-free margins, trauma compromising rib cage integrity, and infectious processes such as chronic osteomyelitis or prosthetic infections. The field has seen significant progress in reconstructive approaches, particularly regarding the materials and techniques employed. Titanium plates, High-Density Polyethylene (HDPE), Polytetrafluoroethylene (PTFE), and biological meshes have reshaped the paradigm, enabling precise, durable, and biocompatible solutions that improve functional outcomes and reduce complications. By highlighting these key advances, this review critically examines transformative developments in chest wall reconstruction, with a focus on innovations in biomaterials, cutting-edge surgical techniques, and personalized technologies such as 3D printing. It also illustrates how these innovations can optimize functional, structural, and aesthetic outcomes for patients with thoracic wall defects.
Keywords: Chest Wall Reconstruction; Thoracic Defects; Technological Innovations
Introduction
Chest wall reconstruction is indicated in cases where thoracic defects compromise structural integrity, respiratory function, or the protection of intrathoracic organs. Defects exceeding 5 cm in diameter, particularly those involving multiple ribs or the sternum, represent a common threshold for reconstruction, as they frequently lead to mechanical instability, respiratory insufficiency, or exposure of vital structures [1,2]. Other indications include thoracic instability caused by flail chest after trauma, resections for malignant tumors requiring clear oncologic margins, and chronic infections such as refractory osteomyelitis or dehiscence of prior surgical repairs. In these scenarios, reconstruction aims to restore anatomical and mechanical stability of the thorax while preventing complications such as lung herniation, chronic pain, and recurrent infections [3]. The decision to perform chest wall reconstruction depends not only on the size and location of the defect but also on clinical factors such as respiratory impact, the potential for progressive decompensation, and the patient’s overall condition. For large or complex defects, achieving an optimal balance between mechanical strength and flexibility is essential to preserve respiratory dynamics and ensure long-term stability. Although the indications for chest wall reconstruction have remained largely consistent over time, prosthetic materials have continued to evolve. A wide variety of materials is now available for reconstruction; however, no single option has been universally accepted as superior. The purpose of this paper is to assess the evolution, use, and outcomes of prosthetic materials in chest wall reconstruction.
Reconstructive Strategies
Reconstructions without Prosthesis
Chest wall reconstruction without the use of prosthetic materials is often indicated in cases of smaller defects, where structural stability can be ensured using autologous tissues, including muscle and fasciocutaneous flaps. Muscle flaps such as the latissimus dorsi, pectoralis major, rectus abdominis, and serratus anterior are widely used to cover bony defects while providing adequate vascularization to the reconstructed area, thereby reducing the risk of infection and promoting tissue regeneration. Reconstruction with autologous flaps provides satisfactory outcomes in patients with localized defects, particularly in cases of chronic infection that contraindicate the use of synthetic materials, (Figures 1A-B). Deschamps et al. reported that the exclusive use of autologous tissues can prevent complications associated with prostheses, such as exposure, migration, and infection, demonstrating high success rates in smaller defects and non-complex resections [1]. However, reconstruction without prosthetic materials is limited in larger defects (>5 cm or involving multiple ribs), as achieving sufficient functional thoracic stability is often difficult and may result in chest wall deformities or compromised ventilation [2].
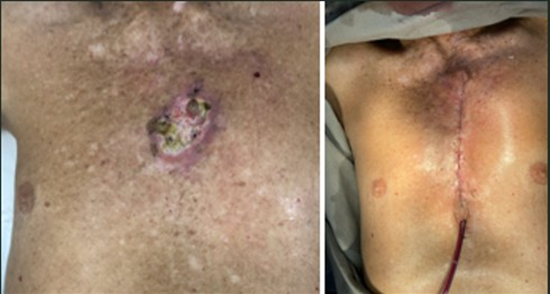
Figure :1 A-B Before And After Reconstruction Without Prosthesis
Polypropylene
Chest wall reconstruction using polypropylene mesh (PPM) is a well-established approach for medium to large defects, particularly in oncologic patients undergoing extensive resections, such as sternectomies or multiple rib resections, (Figure 2). Its success is attributed to favorable mechanical properties, including adequate rigidity for thoracic stability and porosity for tissue integration. Additionally, it is lightweight, easy to handle, and cost-effective [1,2]. The clinical efficacy of this technique was corroborated by de Macedo et al. (2024), who demonstrated that polypropylene mesh in post-sternectomy patients effectively restored thoracic mechanical stability and prevented severe complications such as deformities and respiratory failure. Despite its structural advantages, the main limitation of polypropylene mesh is the increased risk of infectious complications, particularly in contaminated fields or poorly vascularized wounds. To reduce this risk, it is commonly combined with muscle or fasciocutaneous flaps, such as the latissimus dorsi and pectoralis major. These flaps provide robust coverage and additional vascularization, significantly decreasing infection rates [1,4].
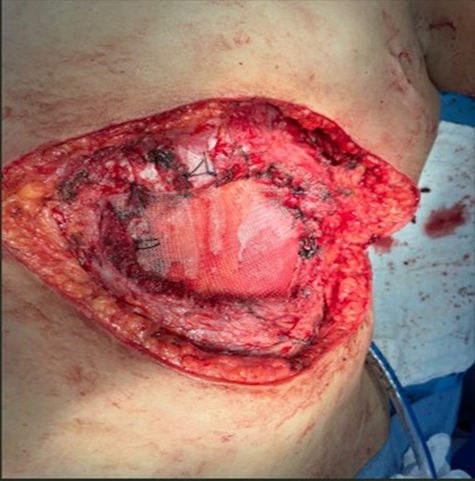
Figure 2: PPM Reconstruction.
Polytetrafluoroethylene (Ptfe)
Polytetrafluoroethylene (PTFE) is a synthetic, non-absorbable, microporous polymer characterized by high biocompatibility, tensile strength, and malleability. Its biological inertness minimizes host inflammatory responses, thereby reducing the risk of infection [5]. The material’s pliability allows precise adaptation to the complex anatomy of the thoracic cage, providing stable structural support without excessive rigidity that could impair respiratory mechanics. Moreover, its impermeability is critical in preventing bronchopleural fistulas and persistent air leaks, which are pivotal to optimizing postoperative outcomes [2]. Clinical literature supports the long-term efficacy and safety of PTFE in chest wall reconstruction. Retrospective analyses and clinical series consistently report low rates of prosthesis-related complications, such as infection, seroma formation, and mechanical failure [1]. Although reconstruction of extensive defects following sarcoma resection presents significant challenges, PTFE has proven effective in enabling radical oncologic resections while restoring functional thoracic integrity [6].
Methyl Methacrylate and Derivative Techniques
Methyl methacrylate is a synthetic polymer widely used in orthopedic and reconstructive surgery due to its excellent mechanical strength, biocompatibility, and moldability. Its ability to rapidly harden into a durable structure while being shaped to anatomical contours makes it particularly suitable for thoracic applications.The use of methyl methacrylate in combination with mesh—commonly referred to as the “sandwich” and “modified sandwich” techniques—has demonstrated favorable outcomes in restoring structural integrity and maintaining pulmonary function. By layering methyl methacrylate between mesh materials, these techniques mimic normal rib biomechanics, providing rigidity while maintaining sufficient flexibility for respiratory movement. The modified sandwich technique further optimizes prosthesis positioning and fixation, reducing displacement risks and improving integration [7]. The neo-rib technique uses molded methyl methacrylate to recreate excised ribs, achieving both functional and aesthetic restoration. The mold is shaped to match anatomical curvature and fixed to adjacent structures with mesh reinforcement. This method effectively reduces paradoxical motion and postoperative pain. Collectively, sandwich, modified sandwich, and neo-rib techniques represent major advancements in modern chest wall reconstruction, offering reliable biomechanical stability and improved quality of life [8].
Titanium Mesh
Titanium meshes have emerged as a key material in chest wall reconstruction due to their high mechanical strength, low weight, and excellent biocompatibility. Titanium’s chemical stability minimizes corrosion and adverse tissue reactions, making it ideal for rigid thoracic prostheses. Tasnim et al. (2023) reported a five-year experience showing a 95% success rate in maintaining pulmonary function, with a low complication rate (7% local infections) and excellent aesthetic results attributed to the mesh’s moldability. Tamburini et al. (2019), in a multicenter study of 62 patients, found that fixation to native bone using screws or stabilization plates provided substantial rigidity, with successful tissue integration in 87% of cases. Postoperative recovery averaged 14 days, and defect recurrence was below 5%. These findings confirm titanium mesh as a highly effective option for large oncologic and complex reconstructions [9,10].
Bone Transplant
Bone grafts, both autografts and allografts, are valued for their biological integration and osteogenic potential. Autologous bone grafts—harvested from the iliac crest, rib, or fibula—are considered the gold standard because of their osteogenic, osteoinductive, and osteoconductive properties, which result in superior integration and reduced rejection risk. Wang et al. (2023) reported a 92.3% success rate in achieving mechanical stability using autologous rib grafts [11]. Allogeneic bone grafts are increasingly used due to availability and reduced donor-site morbidity. Lee et al. (2022) demonstrated comparable mechanical stability to autografts, though with a higher graft resorption rate (14%) [12]. Integration is improved when augmented with biomaterials or bioresorbable fixation plates. The incorporation of 3D printing for anatomical precision further enhances reconstructive outcomes.
3D Printing Technology
Three-dimensional printing has revolutionized chest wall reconstruction by enabling personalized, anatomically precise implants. These technologies improve preoperative planning, reduce operative time, and minimize surgical risks [13]. Improved implant integration and mobility enhance structural stability and respiratory mechanics, leading to better patient satisfaction and faster recovery [14]. Despite these advantages, widespread adoption is limited by high manufacturing costs, regulatory challenges, and the need for specialized expertise [13]. Ensuring long-term biocompatibility and durability remains a critical concern. Ongoing collaboration between engineering and medical disciplines is essential to expand accessibility and optimize production processes [14].
Biological Materials for Chest Wall Reconstruction
Biological materials such as bovine pericardium and acellular dermal matrices are valuable due to their biocompatibility and regenerative properties. Bovine pericardium provides strength, durability, and good tissue integration while reducing rejection risk [15]. Dermal matrices offer flexibility and soft-tissue coverage, making them particularly useful in infected or irradiated fields. Limitations include high cost, variable mechanical strength, and gradual degradation. Bovine pericardium may lose durability over time, while dermal matrices may prolong healing [16,17]. Nevertheless, their immunological compatibility makes them preferred in complex and contaminated cases.
Vitagraft
Vitagraft is a biological scaffold composed of viable autologous fibroblasts and extracellular matrix. It has emerged as a promising option for complex chest wall reconstruction, particularly in radiated or infected fields [18-21]. The prosthesis can be tailored during the procedure, cut with scissors, and molded after immersion in warm saline solution. De Macedo et al. (2025) reported superior biomechanical outcomes and preserved respiratory function following extensive resections. Smith et al. (2023) also demonstrated reduced fistula formation and infection rates, supporting its use in high-risk patients [19]. However, Vitagraft remains limited by high production costs, specialized facilities, and preparation time, which may delay urgent surgery [18,20]. Despite these limitations, it remains a valuable option when conventional materials fail. Future advances in manufacturing may improve its accessibility and cost-effectiveness.
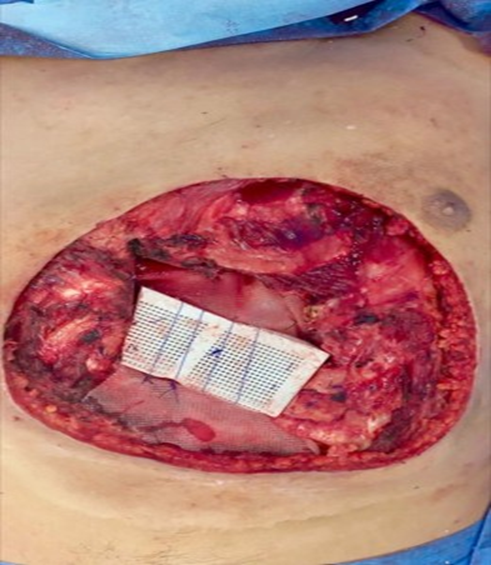
Figure 3: Vitagraft Associated With PPM Reconstruction.
Discussion
The selection of an appropriate prosthetic material for chest wall reconstruction is complex and influenced by multiple factors, including mechanical properties, cost, complication risk, and patient-specific considerations. Reconstructions relying solely on autologous tissues are effective for small and localized defects, providing excellent vascularization and low infection risk. However, they lack sufficient rigidity for large or mechanically demanding defects. Synthetic materials such as polypropylene, PTFE, and methyl methacrylate offer reliable structural support. Polypropylene provides good tissue integration but carries a higher infection risk in contaminated fields. PTFE offers superior biocompatibility but limited rigidity, while methyl methacrylate techniques combine rigidity with respiratory flexibility. Titanium meshes and 3D-printed implants represent advanced solutions for complex reconstructions but are constrained by cost and technical requirements. Biological materials including Vitagraft, bovine pericardium, and dermal matrices offer regenerative properties and low immunogenicity. Vitagraft demonstrates excellent integration and healing, though logistical and financial barriers restrict its broader use. Ultimately, the choice of material must be individualized, considering biomechanical demands, patient condition, and surgical expertise. A tailored approach remains the cornerstone of successful chest wall reconstruction.
References
- Deschamps C, Tirnaksiz BM, Darbandi R, Trastek VF, Allen MS, et al (1999) Early and long-term results of prosthetic chest wall reconstruction. J Thorac Cardiovasc Surg. 117: 588-591; discussion 591-592.
- Chang RR, Mehrara BJ, Disa JJ, Cordeiro PG, Pusic AL, et al (2017) Chest wall reconstruction: an overview. Clin Plast Surg. 44: 571-578.
- Sales JR, Grant TN, Liao J, Chun YS. Early and long-term results of prosthetic chest wall reconstruction. Ann Thorac Surg.
- de Macedo JPC, Nabuco-de-Araujo PHX, Bibas BJ, de Campos JRM, Pêgo-Fernandes PM, et al (2024) Predictors of postoperative complications after sternectomy on oncologic patients. Clinics (Sao Paulo). 79:100468.
- Farid M, Goodwin A, Guo L (2022) Materials and techniques in chest wall reconstruction: a review. J Surg Oncol. 126: 919-929.
- Wald O, Islam I, Amit K, Ehud R, Eldad E, et al (2020) 11-year experience with chest wall resection and reconstruction for primary chest wall sarcomas. J Cardiothorac Surg. 15: 29.
- Weyant MJ, Bains MS, Venkatraman E, Downey RJ, Park BJ, et al (2006) Results of chest wall resection and reconstruction with and without rigid prosthesis. Ann Thorac Surg. 81:279-285.
- Suzuki K, Park BJ, Adusumilli PS, Rizk NP, Huang J, et al (2015) Chest wall reconstruction using a methyl methacrylate neorib and mesh. Ann Thorac Surg.100: 744-747.
- Tasnim S, Betancourt EA, Reyes MM (2024) Five-year experience with titanium mesh for rigid chest wall reconstruction. JTCVS Tech. 28: 180-190.
- Tamburini N, Grossi W, Sanna S, Campisi A, Londero F, et al (2019) Chest wall reconstruction using a new titanium mesh: a multicenters experience. J Thorac Dis. 11: 34593466.
- Wang X, Li H, Zhang R (2023) Outcomes of autologous rib grafts in chest wall reconstruction: a retrospective analysis of 52 cases. J Thorac Cardiovasc Surg. 165:120-128.
- Lee Y, Kim H, Park S (2022) Use of cryopreserved allografts in extensive chest wall reconstruction: A multicenter experience. Ann Thorac Surg. 114: 789-797.
- Smelt J, Pontiki A, Jahangiri M, Rhode K, Nair A, et al (2020) ThreeDimensional Printing for Chest Wall Reconstruction in Thoracic Surgery: Building on Experience. Thorac Cardiovasc Surg. 68: 352356.
- Goldsmith I (2022) Chest Wall Reconstruction With 3D Printing: Anatomical and Functional Considerations. Innovations (Phila). 17:191-200.
- Santos P, Oliveira R, Pereira AC (2023) Advances in the Use of Bovine Pericardium for Chest Wall Reconstruction. Ann Thorac Surg. 115: 455-462.
- Lee H, Kim Y, Park J (2022) Long-term Outcomes of Biological Grafts in Thoracic Wall Reconstruction. Chest. 161:1289-1296.
- Martinez R, Silva P, Gomez L (2023) Role of Acellular Dermal Matrix in Complex Chest Wall Repairs: A Systematic Review. J Cardiothorac Surg. 18: 83.
- De Macedo JPC, Nabuco-de-Araujo PHX, de Campos JRM, PêgoFernandes PM, Terra RM (2025) A new option of reconstruction after extensive chest wall resection. Clinics (Sao Paulo). 80: 100679.
- Smith J, Patel A, Wong T (2023) Clinical Outcomes of Vitagraft in Chest Wall Defect Reconstruction. J Cardiothorac Surg. 18: 123.
- Johnson R, Lee S, Kim Y (2022) Advances in Biological Scaffolds for Chest Wall Repair: Vitagraft Applications. Ann Thorac Surg. 114: 789795.
- Brown P, Garcia R, Lim K (2023) Cost and Resource Challenges in Applying Vitagraft for Thoracic Surgery. Chest.164: 45-51.
© by the Authors & Gavin Publishers. This is an Open Access Journal Article Published Under Attribution-Share Alike CC BY-SA: Creative Commons Attribution-Share Alike 4.0 International License. Read More About Open Access Policy.