Atypical Presentation of A Severe Form of Spontaneous Intracranial Hypotension Due to Multiple CSF Leaks in the Brain and Spinal Cord: Therapeutic Challenge
by Brice Fotsing*, Alionka Bostan, Bernard Dachy
Department of Neurology, Brugmann University Hospital, Université Libre de Bruxelles, Brussels, Belgium
*Corresponding author: Brice Fotsing, Department of Neurology, Brugmann University Hospital, Université Libre de Bruxelles, Brussels, Belgium
Received Date: 06 October 2025
Accepted Date: 10 October 2025
Published Date: 13 October 2025
Citation: Fotsing B, Boston A, Dachy B. (2025). Atypical Presentation of A Severe Form of Spontaneous Intracranial Hypotension Due to Multiple CSF Leaks in the Brain and Spinal Cord: Therapeutic Challenge. 10: 2427. https://doi.org/10.29011/2574-7754.102427
Introduction
Spontaneous intracranial hypotension (SIH) is an uncommon neurological disorder, resulting from spontaneous cerebrospinal fluid (CSF) leakage without identifiable trauma or prior medical procedure. Its presentation is variable and can be atypical, posing diagnostic and therapeutic challenges. Advanced neuroimaging and precise localization of CSF leaks are essential for optimal treatment.
We report a rare and severe case of SIH with multiple CSF leaks at both the skull base and spinal levels, resulting in complex and recurrent symptoms, emphasizing the need for individualized and multimodal management.
Keywords: Spontaneous Intracranial Hypotension; Rhinorrhea CSF; Cerebrospinal Leak At The Base of The Skull; CSF Leak At the Spinal Cord; Meningeal Diverticula
Case Report
A 52-year-old woman with a medical history of chronic obstructive pulmonary disease (COPD), arterial hypertension, dyslipidemia, coronary artery disease, recurrent sinusitis, and surgically treated uterine cancer (no neuraxial anesthesia) presented to our clinic with neurological complaints. She is of slim build, a chronic smoker, and has a persistent cough.
For two months, she had recurrent nocturnal episodes of:
• Orthostatic gait disturbances
• Severe fatigue
• Cognitive disturbances (notably memory lapses)
• A single episode of nocturnal enuresis
• An unusual holocranial headache
These episodes occurred once or twice a month.
Neurological examination revealed bilateral hyposmia. No motor or sensory deficit was noted.
A long-term EEG was normal, excluding epileptic activity.
Brain MRI (Figure 1) revealed:
• Meningeal enhancement in the posterior fossa
• Caudal descent of cerebellar tonsils <5 mm, without evidence of brainstem compression against the foramen magnum.
• Periventricular white matter changes (suggestive of chronic microangiopathy)
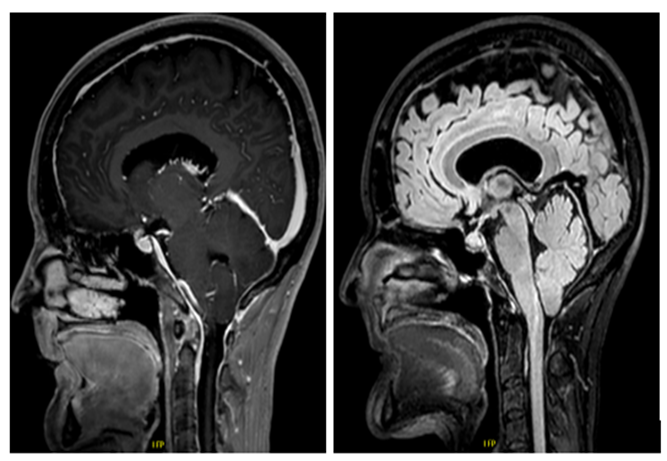
Figure 1: Radiological signs of intracranial hypotension with appearance of pachy-meningitis especially at the posterior fossa and pseudo-chiari with the tonsils in a fairly low position.
To confirm suspected SIH, a lumbar puncture (LP) was performed with the patient in lateral decubitus after prior cranial imaging showed no signs of brainstem compression. The CSF opening pressure was 4 cmH₂O, confirming intracranial hypotension. No contraindications were identified at the time.
Initial treatment consisted of bed rest, hydration, abdominal compression, and a non-targeted lumbar EBP, with no clinical improvement.
Several months later, the patient developed new symptoms:
• Bilateral horizontal diplopia
• Worsening gait ataxia
• Cognitive and behavioral disturbances
• Posterior rhinorrhea
Repeated MRI showed regression of meningeal thickening, a right frontal encephalocele, and multiple thoracolumbar radicular cysts. Spinal imaging with contrast revealed small epidural leaks at L4-L5 and L3-L4 levels (Figure 2).
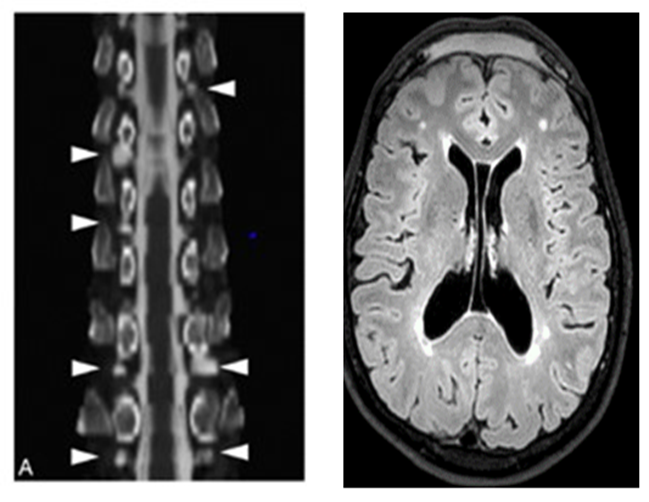
Figure 2: Multiple radicular cysts at the dorsal and lumbar level. Protrusion of the frontal lobe at the level of the crista galli on the right corresponding to a right encephalocele.
A radioisotope cisternography confirmed:
• Persistent low CSF pressure (4 cmH₂O)
• CSF leak at D12 and L3
• CSF rhinorrhea confirmed by tracer in nasal secretions at the cribriform
Treatment included:
• A targeted thoracolumbar EBP
• Surgical repair of the skull base defect was performed via a transcranial approach through a bifrontal craniotomy, allowing exploration of the skull base and cribriform plate. A periosteal graft was meticulously positioned to seal the cerebrospinal fluid leak, with careful preservation of adjacent olfactory and vascular structures. This approach enabled direct access to the encephalocele while minimizing disruption to surrounding tissues.
The surgery was complicated by a right parietal subdural collection, associated with transient left-hand paresis.
Postoperative evolution was marked by:
• Partial and transient improvement
• Persistence of chronic exertional headaches (triggered by cough and effort)
• Recurrence of anterior and posterior rhinorrhea
• Persistent memory impairment
Postoperative imaging (MRI and CT scans) confirmed the persistence of CSF leak at both the cribriform plate and thoracolumbar levels (Figure 3). Isotope cisternography likewise showed residual tracer accumulation at these sites. Connective tissue disorders were ruled out.
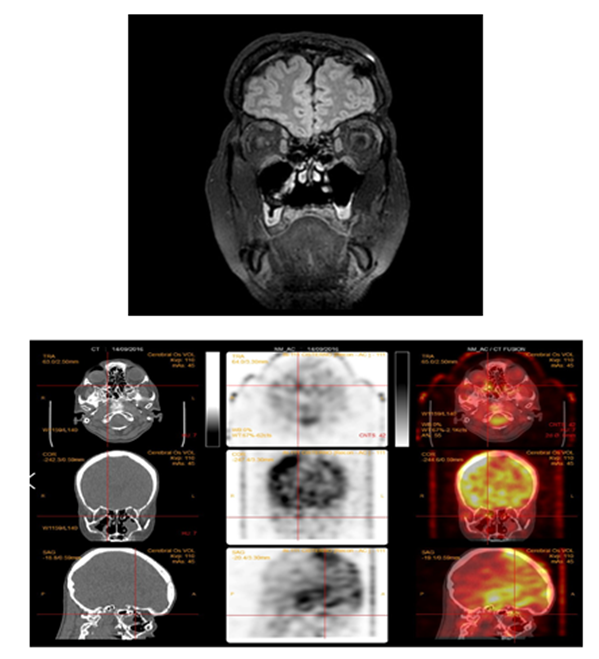
Figure 3A: Postoperative MRI shows the encephalocele and the periosteal graft sealing the CSF leak at the right paramedian cribriform plate. B: Isotopic cisternography with CT fusion demonstrates persistent CSF leakage at the cribriform plate and at the spinal cysts.
Discussion
This case illustrates a rare and severe form of SIH with multiple CSF leaks, both cranial (encephalocele and rhinorrhea) and spinal (radicular cysts). Such dual-location leaks are exceptional and make diagnosis and management difficult.
According to ICHD-3 criteria, SIH diagnosis requires:
• Headaches temporally related to low CSF pressure or a leak
• CSF-OP < 6 cmH₂O
• Compatible imaging findings [1, 2]
Four clinical forms of SIH are theoretically described [3].
This patient exhibited an atypical form (type IV SIH).
Our patient had both a frontal encephalocele and spinal meningeal diverticula, which are known to be associated with SIH, particularly in the absence of connective tissue disorders [4]. The risk of performing LP in the presence of cerebellar tonsillar descent is well known. However, pre-procedural MRI showed no signs of active brainstem compression, and the LP was necessary to confirm the diagnosis and guide treatment.
Cranial CSF leaks especially through encephaloceles can mimic or coexist with SIH and may be primary or secondary to raised intracranial pressure [5].
Management remains empirical:
• Initial conservative therapy (hydration, caffeine, abdominal binders)
• Repeated empirical lumbar EBP (first-line intervention)
• Targeted EBP guided by imaging in case of identified leaks
• Surgical closure of cranial and/or spinal leaks when refractory
Despite surgical repair of the cranial CSF leak and targeted EBP, the patient experienced symptom recurrence, including persistent rhinorrhea, exertional headaches, and cognitive impairment. Contributing factors may include residual leaks at the cribriform plate and lumbar root sleeves, postoperative complications such as parietal subdural collection affecting healing, mechanical factors like chronic smoking and coughing increasing intracranial pressure, and incomplete therapeutic responses due to multifocal leak sites.
This case highlights the limitations of current therapeutic approaches, especially in multifocal leaks with partial or no long-term response.
Conclusion
SIH is an often underdiagnosed condition, particularly in atypical or non-orthostatic presentations. This case emphasizes the diagnostic and therapeutic challenges of SIH with both cranial and spinal CSF leaks. Our case demonstrates the need for comprehensive imaging, individualized therapeutic strategies, and multidisciplinary management, especially in the presence of multiple and persistent leaks.
Despite surgical and interventional efforts, some patients may experience chronic disabling symptoms, underlining the need for more robust therapeutic protocols and prospective studies. A multidisciplinary approach and long-term follow-up are essential.
Abbreviations: CSF: Cerebrospinal fluid; CSF-OP: CSF opening pressure; SIH: Spontaneous intracranial hypotension; EBP: epidural blood patch; COPD: Chronic obstructive pulmonary disease
Conflicts of interest
Authors have nothing to declare.
Funding
None.
Data availability
The data that support the findings of this study are available on request from the corresponding author, SB. The data are not publicly available due to their containing information that could compromise the privacy of research participants.
Author contributions
BF: conceptualization, data curation, formal analysis, investigation, methodology, project administration, software, validation, visualization, writing – original draft, writing – review & editing. AB: data curation, investigation, software, visualization. BD: project administration, resources, supervision, validation, visualization, writing – review & editing.
References
- Schievink WI. (2021). Spontaneous Intracranial Hypotension. N Engl J Med. 385: 2173-2178.
- Headache Classification Committee of the international Headache Society. The international classification of headache disorders, 3rd edition. Cephalalgia 2018; 38: 1-211.
- D’antona L, Jaime Merchan MA, Vassillou A. (2021). clinical presentation, investigation findings and treatment outcomes of spontaneous intracranial hypotension syndrome : a systematic review and meta-analysis. JAMA Neurol. 78: 329-337.
- Kranz PG, Stinnett SS. (2013). Spinal Meningeal diverticula in spontaneous intracranial hypotension: analysis of prevalence and myelographic appearance. AJNR Am J Neuroradiol. 34: 1284-1289.
- Schievink WI, Michael LM II, Maya M, Klimo P Jr, Elijovich L. (2021). Spontaneous intracranial hypotension due to skull-base cerebrospinal fluid leak. Ann Neurol. 90: 514-516.
© by the Authors & Gavin Publishers. This is an Open Access Journal Article Published Under Attribution-Share Alike CC BY-SA: Creative Commons Attribution-Share Alike 4.0 International License. Read More About Open Access Policy.